Investigators in the Metabolic Epidemiology Branch (MEB) conduct a synergistic, cutting-edge prostate cancer research program focused on increasing our understanding of the causes of this cancer as well as discovering and validating predictive biomarkers for clinical translation. Central themes include endogenous and exogenous sex steroid hormones, micronutrients and vitamin supplementation, reproductive factors, tissue-based biomarkers, and metabolomics, as well as examination of other population differences.
By focusing on identifiable subsets of clinically-relevant prostate cancer (e.g., aggressive and lethal forms), MEB investigators seek to differentiate clinically relevant disease and avoid dilution of associations by indolent prostate cancers. They use state-of-the-art methods and novel approaches, drawing upon the distinct features of the Intramural Research Program at the NIH and collaborating with expert extramural groups around the world.
Prostate Cancer Research Areas
Prostate Cancer Trends and Racial Differences
MEB investigators continue to study prostate cancer trends and the basis of racial differences in this disease. Recent studies include U.S. incidence trends of lethal prostate cancer, U.S. current trends and future projections of metastatic prostate cancer, and international trends in prostate cancer incidence. They are making full use of the Ghana Prostate Study, the Prostate, Lung, Colorectal and Ovarian (PLCO) Trial, the Alpha-Tocopherol, Beta-Carotene Cancer Prevention (ATBC) Study, AARP Diet and Health Study, and other intramural/extramural resources and collaborations to study racial differences in prostate cancer risks, assessing questionnaire data, germline genetics, serum, and tissue. Black-white differences in prostate cancer risk factor profiles were found for height and vitamin D intake, whereas lower risk in diabetic men was common to both races. The recently formed Prostate Cancer Cohort Consortium (PC3) within the NCI Cohort Consortium will provide additional collaborations to further their assessments of racial differences in prostate cancer risks.
Micronutrients and Vitamin Supplementation
MEB investigators have aggressively pursued the etiologic role of vitamins D, E and A in prostate cancer. Their studies of vitamin D include measurement of both the accepted biomarker of vitamin D status, 25-hydroxy-vitamin D [25(OH)D], and its major carrier protein, vitamin D binding protein (DBP). A large investigation in the ATBC Study showed significantly elevated risk among men with higher circulating vitamin D, which is now an accepted association supported by analyses of vitamin D genetic variants and polygenic scores from genome-wide association studies (GWAS). By contrast, higher vitamin D status is associated with improved prostate cancer survival. Investigators are examining biological mechanisms through cross-sectional analyses of hormones in the National Health and Nutrition Examination Survey (NHANES) and through ChIP-Seq cell culture functional experiments testing the effect of exposure to vitamin D and DHT on key nuclear receptors (i.e., AR, VDR, RAR/RXR) and gene regulation.
The 32% reduction in prostate cancer incidence in the α-tocopherol (50 IU/day) arm of the ATBC Study was the basis of investigators' research into vitamin E. Their lines of inquiry focus on dose levels, smoking status, tocopherol fractions, mechanisms, and cancer stage, as well as whether genetic variants contributing to vitamin E status play some role. In the Selenium and Vitamin E Cancer Prevention Trial (SELECT) trial, higher prostate cancer incidence in men receiving 400 IU of vitamin E daily raised questions concerning supra-physiological supplementation and cancer stage-specific mechanisms for vitamin E and other micronutrients. Investigators have shown improved 20-year survival in cases with higher baseline vitamin E status and those receiving the ATBC 50 IU dose, and an impact of vitamin E on androgens and vascular endothelial growth factor (VEGF) consistent with tumor growth inhibition. They have also shown a direct association between circulating retinol and prostate cancer risk in their studies and in the EHNPCCG consortium.
Metabolomics
Metabolomic profiling is a relatively new laboratory methodology that simultaneously measures thousands of low molecular weight biochemicals (i.e., <1kDa) in blood and other biospecimens. MEB investigators have conducted untargeted studies of prostate cancer risk, similar to other agnostic, “broad spectrum” research approaches such as GWAS, to discover biologically-based etiologic metabolites. Their initial investigations have identified strong lipid signals, including glycerophospholipids, sphingomyelins, and inositols, related to aggressive and lethal prostate cancer. By contrast, they found N-oleolyltaurine and androgens associated with prostate cancer survival, and have leveraged these studies to examine overall and cause-specific mortality.
Sex Steroid Hormones and Reproductive Factors
MEB investigators have conducted various studies of sex steroid hormones, reproductive factors, and prostate cancer. For example, they have provided evidence that the estrogen-androgen balance may be important in the development of aggressive prostate cancer and they have provided evidence that circulating measures of sex steroid hormones may be poor proxies of the intraprostatic milieu. Investigators continue to assess other proxies of sex steroid hormones such as male pattern baldness (androgenic alopecia), vasectomy, infertility, sexually transmitted infections as well as assessment of methods to quantitate sex hormones in formalin-fixed, paraffin-embedded prostate biopsy tissues. They have worked closely in collaboration with the Endogenous Hormones, Nutritional Biomarkers and Prostate Cancer Collaborative Group (University of Oxford, U.K.) to discover multiple new findings of prostate cancer etiology through the combined statistical power of more than a dozen cohorts, investigating the role of hormones, growth factors, diabetes, and micronutrients. They are also interested in the effects of exogeneous testosterone on prostate cancer risk.
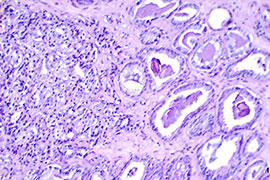
Tissue-based Markers for Prognostication
TMPRSS2-ERG brings together an androgen-responsive promoter (TMPRSS2) and an oncogene (ERG), resulting in overexpression of a functional chimeric ERG protein. MEB investigators have assessed this gene fusion—which is observed in a significant number of prostate cancers—in the Ghana Prostate Study as well as in a systematic review and meta-analysis to assess racial differences. Negative ERG staining was associated with higher Gleason score in Ghana, while the meta-analysis showed the prevalence of TMPRSS2-ERG fusions in prostate cancer to be highest in men of European descent (49%) followed by Asian (27%) and then African (25%). Investigators are currently conducting studies of intra-prostatic cell cycle proteins and mitotic tissue proteins in relation to the risk of prostate cancer recurrence in the PLCO study. They are also currently conducting studies of computational pathology in an attempt to improve prognostic algorithms.
Selected Studies
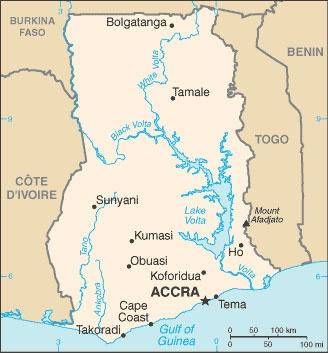
The Ghana Prostate Study
The Ghana Prostate Study is designed to assess the burden, risk factor profiles and biomarkers of prostate cancer in Ghanaian men. In the United States, incidence rates of prostate cancer in African-Americans are 1.6-fold higher than those observed in European Americans, yet the causes of this difference remain unknown. Since West Africa is the principal ancestral origin of a substantial proportion of African-American men, one may hypothesize that genetic susceptibility loci that vary in allele frequency by ancestral population could account for part of the observed differences in prostate cancer rates within the U.S. In addition, little is known about the prostate cancer risk factors in African men. Read more about the Ghana Prostate Study.
Prostate Cancer in the Alpha-Tocopherol, Beta-Carotene Cancer Prevention (ATBC) Study
The ATBC Study has been an integral male cohort research resource for NCI for nearly three decades. The trial was designed to test hypotheses based on epidemiological and experimental evidence supporting nutritional prevention of cancer, and tested supplementation with β-carotene (20 mg/day) and vitamin E (50 mg/day, as dl-α-tocopheryl acetate) for 5-8 years in 29,133 male smokers (>5 cigarettes daily), finding a 32% and 40% reduction in prostate cancer incidence and mortality, respectively, in the vitamin E arm. Currently, 2,900 prostate cancers have been ascertained and serum etiologic studies have focused on growth factors, insulin, thyroxine, sex hormones, vitamins D, E, and A, and metabolomic profiling. ATBC has actively contributed to several prostate cancer consortia including BPC3, EHNPCCG, and PRACTICAL. The study has published nearly 100 prostate cancer research studies.
Prostate, Lung, Colorectal and Ovarian (PLCO) Cancer Cohort Study
The PLCO Study enrolled 76,683 men aged 55 to 74 years during 1993–2001 from ten cancer screening centers across the United States. For the prostate component, men were randomly assigned to usual care with opportunistic screening or to annual screening with prostate-specific antigen (PSA) testing at baseline and for a further six years (with optional annual digital rectal exam at baseline and for a further four years). Participants were followed for incident cancer diagnoses and cause-specific mortality. All men were uncompensated volunteers from the general population with no prior medical history of any cancer (except nonmelanoma skin cancer). Men were excluded for prior removal of their prostate gland, participation in another cancer screening or prevention trial, Finasteride use within six months prior to enrollment, and—starting in 1995 after a study protocol change—if they had received more than one PSA test in the three-year period prior to enrollment. MEB investigators have leveraged this prospective cohort study to test various hypotheses related to prostate cancer pathogenesis and prognosis, including assessment of questionnaire data, baseline and follow-up blood samples, and tissue microarrays for a subset of men who underwent radical prostatectomy.