Meredith Shiels, Ph.D., M.H.S.
NCI Shady Grove | Room 6E104
Biography
Dr. Meredith Shiels earned her M.H.S. and Ph.D. in cancer epidemiology from the Johns Hopkins Bloomberg School of Public Health. She joined the Infections and Immunoepidemiology Branch (IIB) as a Cancer Research Training Award postdoctoral fellow in 2009 and was promoted to research fellow in 2011. She became a tenure-track investigator in 2016 and was promoted to senior investigator and awarded NIH scientific tenure in 2021. Dr. Shiels's has been recognized with may honors and awards including the Sallie Rosen Kaplan Fellowship for Women Scientists in Cancer Research in 2009, the DCEG Women Scientist Advisor’s Mentoring and Leadership Award in 2020 and the DCEG Outstanding Mentor Award in 2025. In 2024, she was elected to a three-year term as a DCEG Women Scientist Advisor.
Research Interests
Dr. Shiels uses innovative approaches to confront high-impact public health questions with population-based data resources and descriptive analyses. She combines multiple population-based data resources, quantifies the contribution of risk factors to time trends, and disaggregates cancer incidence and mortality rates to reveal underlying patterns and explanatory mechanisms. Currently, her research program focuses on 1) quantifying cancer risk and burden in people with HIV, 2) estimating the impact of risk factors on changing cancer rates over time, and 3) providing insights into emerging public health crises in the United States.
Dr. Shiels's Research Team
Dr. Shiels's research team includes the following fellows:
- Cameron B. Haas, Ph.D., M.P.H., Postdoctoral Fellow
- Jennifer McGee-Avila, Ph.D., M.P.H., C.H.E.S., C.P.H., Postdoctoral Fellow
- Wayne Lawrence, Dr.P.H., M.P.H., Research Fellow, Metabolic Epidemiology Branch
- Beth Maclin, Ph.D., M.P.H., Postdoctoral Fellow
Cancer Risk and Burden in People with HIV
Cancer is a significant comorbidity among people with HIV and understanding the shifting landscape of cancer risk and burden has public health implications for prevention and the allocation of both research and resources. Dr. Shiels’s work among people with HIV quantifies the evolving epidemiology of cancer, provides insight into cancer etiology, and examines the association between HIV and cancer progression. Dr. Shiels is the co-principal investigator of the HIV/AIDS Cancer Match Study, a data linkage study of population-based HIV and cancer registries in the United States. Her recent work has estimated the contribution of HIV to rising anal cancer rates in the U.S. general population, and that the absolute risk of lung cancer among older people with HIV is greater than the risk of Kaposi sarcoma or non-Hodgkin lymphoma.
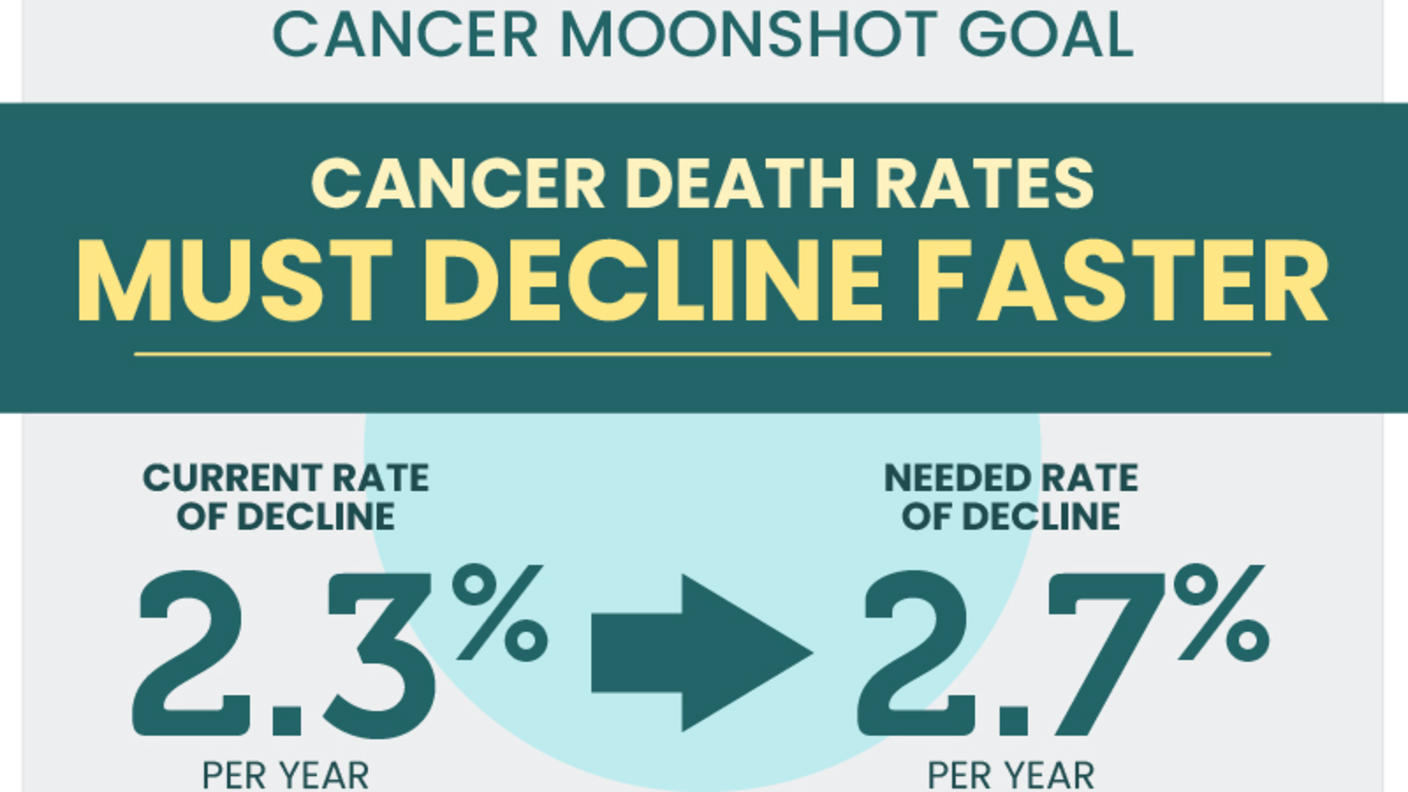
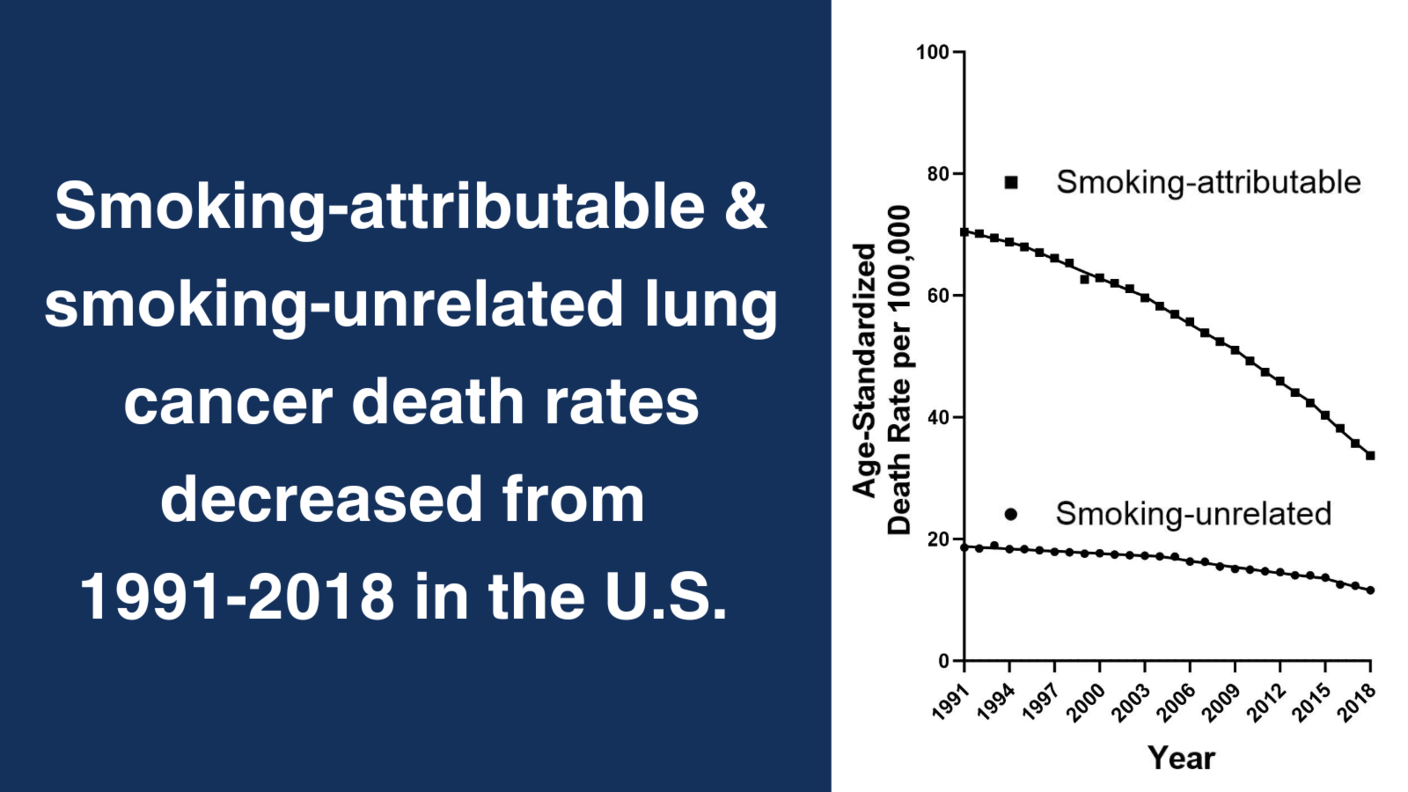
The Impact of Risk Factors on Trends in Cancer Rates
Dr. Shiels’s research program characterizes the extent to which candidate risk factors are driving observed temporal increases or decreases in cancer incidence rates. As cancer registries generally do not collect risk factor data, she uses linked databases and statistical modeling to disaggregate rates based on etiology, which is important for targeted prevention efforts. In recent studies, Dr. Shiels estimated the role of hepatitis C and hepatitis B viruses in rising rates of hepatocellular carcinoma, and the impact of the increasing prevalence of overweight and obesity on rising rates of papillary thyroid cancers.
Providing Insights into Emerging Public Health Crises
Dr. Shiels additionally has applied her expertise in interrogating large, population-based data to address emerging public health questions related to the underlying drivers of premature mortality (deaths among 25-64-year-olds) rates in the United States. Some of this work has focused on the evolving drug overdose epidemic, which is a main contributor to rising premature mortality rates in some groups. In 2020, Dr. Shiels expanded her research program to include descriptive analyses of COVID-19. She has estimated excess death rates in the U.S. during the COVID-19 pandemic, showing the importance of accounting for population growth and aging in excess death calculations and highlighting profound racial/ethnic disparities in excess deaths during the pandemic.
Information for Journalists
To request an interview with a DCEG investigator, please complete this form: Request For Comment | HHS.gov.