Collaborations Around the World: DCEG Research in Latin America
, by Jennifer K. Loukissas, M.P.P.
Studies in Latin America have allowed us to develop data-rich and well-powered studies to further our understanding of cancer risks among Latino individuals in the U.S. and to inform prevention efforts at home and abroad.
Research projects in the Division of Cancer Epidemiology and Genetics (DCEG) span the globe. While many studies are conducted in the United States, partnerships with researchers across Latin America (Mexico, Central and South America, and the Caribbean) have allowed DCEG scientists to develop data-rich and well-powered studies to investigate often highly lethal cancers that occur with lower frequency in the U.S., better understand cancer risks among Latino individuals in the U.S., and inform prevention efforts at home and abroad.
A Note About Language
There are several ways to refer to a person who traces their roots to Latin America. For this article, we use Latino to refer to these populations. The word Hispanic describes individuals who trace their roots to countries whose primary language is Spanish, which includes many countries in Latin America.
A growing number of Americans identify as Latino. Overall cancer incidence and mortality, as well as death from all causes, are lower for these populations compared to other racial and ethnic groups. While studies within the U.S. can provide meaningful insights into these patterns, the proportion of Latino individuals within existing studies is small, thus limiting research opportunities. An investigation into premature mortality conducted by Yingxi Chen, M.D., Ph.D., staff scientist in the Metabolic Epidemiology Branch (MEB), and colleagues, compared data from the U.S. with 12 Latin American countries. They identified evidence to support what has been termed the ‘Latino Paradox’: health status and health outcomes more favorable than disadvantageous socioeconomic factors would suggest. This research has expanded our understanding of the health of populations across Latin America and in the U.S.
“Collaborations across the continents have afforded us the opportunity to identify potential risk factors and better understand the etiology of numerous cancer types. We look forward to continued progress with our partners in Latin America,” said Stephen J. Chanock, M.D., Director, DCEG. “In many of the studies described below, DCEG investigators are contributing to the body of evidence needed to inform policies, clinical practice, or regulations to improve public health; for example, studying new screening protocols or testing potentially contaminated foodstuffs.”
Collaborating with New and Existing Cohorts
While cohorts and other study populations in the U.S. are not well-powered enough to study cancer and other outcomes among Latino individuals, large studies in Latin America aiming to address the research gaps are in early stages. DCEG investigators have been involved in launching some of these studies, which will be discussed later in this article.
In MEB, Emily Vogtmann, Ph.D., M.P.H., and Erikka Loftfield, Ph.D., M.P.H., Earl Stadtman investigators, and Rashmi Sinha, Ph.D., senior investigator, have begun collaborating with the leaders of the Mexican Teachers Cohort Study (MTC), part of the NCI Cohort Consortium. MTC began in 2006 and includes 115,306 women teachers in 12 states in Mexico. Participants have been followed over time for mortality outcomes, and recently, investigators have been validating methods for linkage to health insurance databases to identify incident cancers and other outcomes.
This partnership will allow MEB scientists to study multiple exposures, including diet and tobacco use, and cancer risk and mortality within Mexican women, and compare them to patterns in U.S.-based cohorts. MTC is currently evaluating the feasibility of collecting oral and fecal samples for microbiome studies. Collecting samples from this cohort would help ensure diverse representation in future microbiome studies.
Going Where the Cancer Incidence is High
Many of the most fatal cancers in the U.S. are also some of the rarer types. In order to develop prevention strategies and early detection methods, we need a better understanding of their causes. Thus, DCEG investigators seek collaborations in places around the world where incidence of certain malignancies is high to facilitate studies of their etiology.
Gallbladder (Biliary) Cancer in South America
In Chile, incidence and mortality from gallbladder cancer are among the highest in the world. While gallbladder cancer does have at least one well-established risk factor—gallstones—the rate of gallbladder cancer among individuals with gallstones is low and removing the gallbladder (the main treatment for gallstones) has risks.
Jill Koshiol, Ph.D., senior investigator in the Infections and Immunoepidemiology Branch (IIB), launched the Chile Biliary Longitudinal Study (Chile BiLS), a cohort of women with gallstones, to describe a risk profile for patients more likely to progress to gallbladder cancer and to investigate the etiology of this highly fatal malignancy. Women were chosen as the population of interest because gallbladder cancer is more common in women than in men. The study is conducted in collaboration with experts at the Pontificia Universidad Católica de Chile and the Universidad de la Frontera.
“Our work has led to the identification of a novel association between aflatoxin and gallbladder cancer,” said Dr. Koshiol. “These findings prompted the Chilean government testing of merkén, a spice blend that might be contaminated with fungal toxins like aflatoxin.” The government recalled one brand with high levels of contamination and issued a food safety warning.
The multidisciplinary team is in the process of completing a descriptive analysis of gallbladder cancer mortality trends and how they might have been impacted by new universal healthcare coverage policies in Chile. Ongoing and planned analyses include the investigation of epidemiologic risk factors, characterization of immune features, and the creation of risk prediction models.
Dr. Koshiol has also helped to launch the Maule Cohort (MAUCO), which began in 2014 with the goal of prospectively evaluating cancer and cardiovascular disease in central Chile. She has since conducted some studies of gallstones within this population and will compare the male participants with gallstones to the Chile BiLS cohort.
Stomach (Gastric) Cancer
The distribution of stomach cancer burden around the world is uneven. Several Asian and Latin American countries experience particularly high incidence rates and, in the U.S., minoritized populations, including Asian and Hispanic/Latino individuals, have an increased risk of developing and dying from stomach cancer compared with non-Hispanic White individuals. For this reason, descriptive, genetic, and other epidemiological studies to understand the causes of stomach cancer are being carried out in Latin America.
Maria Constanza Camargo, Ph.D., Earl Stadtman investigator, MEB, and colleagues studied stomach cancer mortality trends in Hispanic/Latino populations in the U.S., Puerto Rico, and 16 Latin American countries. They observed declining stomach cancer mortality rates in the last two decades. However, there was a notable variation in trends by country, sex, and age group, emphasizing that continued and targeted prevention efforts are needed to reduce the disease burden in these vulnerable populations.
Studies to Inform Stomach Cancer Prevention and Early Detection
“There is no standard or routine screening for stomach cancer in Latin America,” said Dr. Camargo. “We are collaborating with a network of Latin American colleagues to identify approaches for risk stratification and prevention strategies through the Gastric Cancer Precursor Lesions (GCPL) Study.”
The GCPL Study evaluates risk factors and potential noninvasive screening markers for intestinal metaplasia, a precancerous transformation of the mucosal lining of the stomach to intestinal epithelium that confers an increased risk of stomach cancer. A better understanding of stomach cancer etiology may inform future efforts for prevention and control in the U.S. and globally.
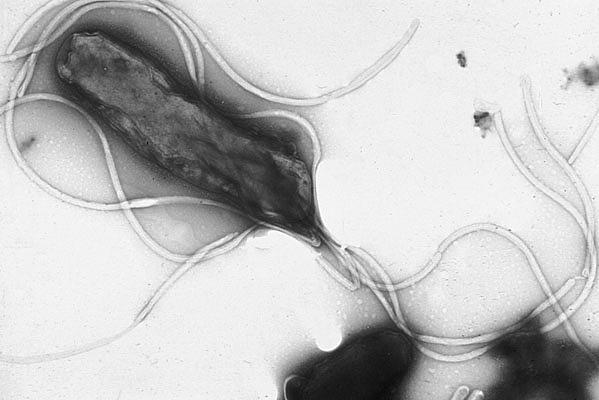
Understanding a Bacterial Carcinogen
A major contributor to stomach cancer risk is infection with the bacterium Helicobacter pylori (H. pylori). The H. pylori Genome Project (HpGP), a large-scale biobank of ~1000 clinically annotated strains, is underway with the first publication expected this year. HpGP is jointly led by Dr. Camargo and Charles Rabkin, M.D., senior investigator in IIB. “Genetic analyses of H. pylori strains from North, Central, and South America are revealing some unique features, as compared to bacterial isolates from other parts of the world,” said Dr. Rabkin. “The open-access data generated in the HpGP will facilitate understanding of the pathophysiology and clinical implications of chronic H. pylori infection.”
Identifying Genetic Susceptibility
Emerging genome-wide association study (GWAS) data from populations of non-European ancestries are making important contributions toward understanding carcinogenesis. For stomach cancer, in collaboration with more than 20 institutions, Dr. Camargo is leading a GWAS in Hispanic/Latino populations to identify susceptibility genetic variants for etiologic insights and better estimates of disease heritability. The study includes ~3500 stomach cancer cases and ~5000 controls from Brazil, Chile, Colombia, Guatemala, Honduras, Mexico, Peru, and the U.S.
Liver Cancer: A Cancer Moonshot Priority
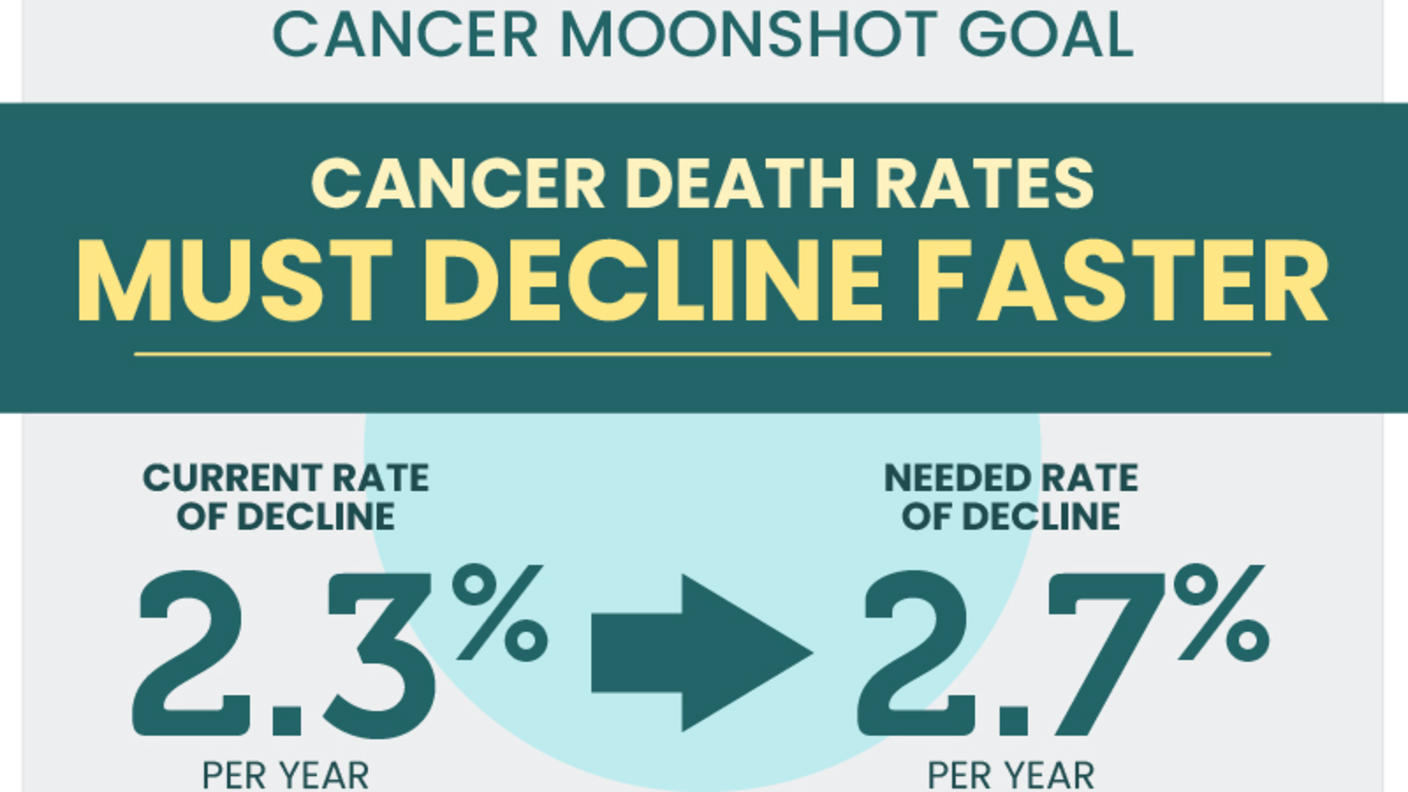
Liver cancer is the sixth most commonly occurring cancer in the world, and, due to a very poor prognosis, it is the third largest contributor to cancer mortality. In the U.S., incidence rates are more than two-fold higher among Hispanic/Latino individuals compared to non-Hispanic White individuals. The Cancer Moonshot℠ identified liver cancer as one of the six cancers that require considerable progress to meet the goal of lowering the age-adjusted cancer mortality rate by 50%.
Guatemala has the highest incidence and mortality rates of liver cancer in the western hemisphere and, unlikely many countries, the rates are very similar among women and men. Katherine A. McGlynn, Ph.D., M.P.H., senior investigator, MEB, is partnering with researchers in Guatemala to better understand how the unusual incidence patterns relate to known and novel risk factors. Factors being studied include hepatitis B and hepatitis C virus infections, aflatoxin and other mycotoxin exposures, metabolic conditions, and non-alcoholic fatty liver disease. To pursue the leads previously identified by the investigators in cross-sectional studies, they are currently conducting a case-control study in collaboration with the Institute of Nutrition of Central America and Panama, headquartered in Guatemala City. Read more about the North American Liver Cancer Study.
Accelerating Control of Cervical Cancer, a Leading Cause of Cancer Death in Women
Despite the existence of effective cervical cancer prevention (HPV vaccines), screening, and treatment modalities, there were over 600,000 cases of cervical cancer worldwide in 2020 and approximately 342,000 deaths; 90% of these deaths occurred in low- and middle-income countries. For over 30 years, researchers in DCEG have been collaborating with clinicians and researchers in Costa Rica in areas where prevalence and death from cervical cancer was high. This partnership has yielded much of what we know about the natural history of HPV infection and cervical cancer and served as the home for the Costa Rica HPV Vaccine Trial (CVT), led by Aimée R. Kreimer, Ph.D., senior investigator, IIB. CVT is the only pre-licensure government-funded double-blinded randomized controlled clinical trial, which led to the discovery that one dose of the HPV vaccine might provide adequate protection over a decade after initial vaccination. Given the potential public health implication of these findings, several new single-dose HPV vaccination trials were launched, including the ESCUDDO Efficacy Trial, a part of the Cancer Moonshot Initiative.
The PAVE Consortium Project was established by Mark Schiffman, M.D., M.P.H., senior investigator, Clinical Genetics Branch (CGB), and colleagues, to test new cervical cancer prevention approaches using HPV testing and automated visual evaluation in various locations across Central and South America and other regions of the world with limited resources and access to screening. These interventions include novel sample collection methods; HPV genotyping assays for studies of natural history; vaccination, screening, and management programs; and low-cost tests to triage HPV-positive individuals. Similarly, Nicolas Wentzensen, M.D., Ph.D., M.S., deputy director and senior investigator, CGB, and Megan Clarke, Ph.D., M.H.S., Earl Stadtman investigator, CGB, are evaluating novel triage tests like automated dual stain and HPV methylation in various places around the world including the Caribbean. Learn more about these efforts to control cervical cancer.
Smaller Scale Projects
In addition to larger-scale collaborations that span many years or even decades, smaller projects can provide important evidence to the broader scientific community. In partnership with clinical colleagues at universities and hospitals in São Paulo, investigators in the Radiation Epidemiology Branch are evaluating risk of dying from a second cancer among patients with retinoblastoma in Brazil. Initial findings suggest that patients in Brazil were frequently diagnosed at a more advanced stage of the disease than patients in the U.S. The investigators hope results from this work can provide valuable perspectives on issues related to early diagnosis, treatment, and long-term clinical care.
The fruitful partnerships described here enrich our research program. Not mentioned are our considerable collaborations with our neighbor to the north, Canada. The breadth and depth of our connections with Canada will be described in a future article.